The Northwest Territories Health and Social Services Authority (NTHSSA) on Friday outlined what it would do in case an outbreak or multiple outbreaks of Covid-19 occur in the fall.
"The hardest is yet to come with Covid in the NWT," said outgoing territorial medical director Dr. Sarah Cook, who presented the plan to reporters during a video conference.
While the plan isn't new for people working in the NWT's health-care system, Cook said, the NTHSSA decided to release it to the public now because the season of wider spread respiratory illnesses is approaching as students return to school and more people return to work.

GNWT image
The purpose of the plan is to build confidence in the health care response to the pandemic, inform the public what it can expect from the perspective of patient care and help NWT residents understand the capacity of the health-care system as it faces the pandemic, the NTHSSA said in a separate press release.
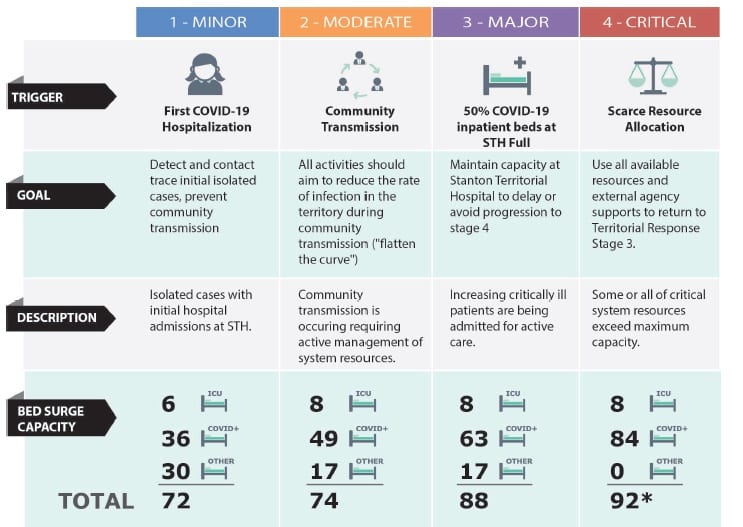
The plan structures its pandemic response according to four stages of outbreak severity.
In the first stage, referred to as "minor" in the plan, there are isolated cases of Covid with initial admissions to Stanton Territorial Hospital. Resources are reallocated and non-essential services are reduced.
Detecting and contact tracing is mobilized, community transmission is prevented through actions by the Office of the Chief Public Health Officer and in-person healthcare interactions are reduced by replacing them with virtual care, where appropriate.
"We were in that stage a few months ago," Cook said.
In stage two, or "moderate," there is community transmission of Covid. Resources must be actively managed to respond to rising needs as more people are admitted to Stanton. Delays of critical patient transfers should be expected.
NTHSSA image
All efforts must be made to reduce the spread and maintain sustainability of resources and delay the progression to the third stage.
The third, or "major" stage involves facing increasing numbers of critically ill patients being admitted to Stanton for active care. Some patients with moderate symptoms would be sent to Inuvik Regional Hospital. It is possible some would be moved out of the territory by medevac. It is expected that 50 per cent of the 100 inpatient beds at Stanton would be full, and early discharges would be the goal to keep more inpatient beds available. Any external resources available would be prepared for activation.
The fourth stage, "critical," has some or all of the health care resources in the NWT operating above capacity. Scarce resource allocation decisions would be needed, with all resources and external agency supports used to return to the third stage as quickly as possible.
Partnerships with the Alberta health care system would be accessed to secure more resources, if needed, such as machines that pump oxygen into a patient's bloodstream. There are no such devices in the NWT, Cook said.
Where necessary, additional staff would be added to the health-care system or reallocated as required, including moving staff to other communities.
Moderate symptoms
The plan states that 80 per cent of people who test positive for Covid will have mild symptoms. They will stay at home if they can self-isolate and will be visited by a health-care provider or receive virtual assessments.
If their condition worsens, patients will be offered care based on symptom severity and goals of care, based on a patient's values when they have a severe illness. If they choose comfort care, or palliative care, it will be provided at Stanton, Inuvik Regional Hospital or and Hay River Regional Health Centre.
Maintaining health care during outbreaks
Non-Covid-related health services care would still be offered during outbreaks, but Cook said that a proper balance must be found.
"Non-urgent care, such as elective surgeries, would be ramped down," she said, referring to how those surgeries were postponed in the spring. But urgent care would be maintained.
To manage resources, face-to-face health encounters would shift to virtual encounters over the phone, by video or secure messaging; and patient movement would be reduced by decreasing unnecessary trips to to health care facilities.
Cook emphasized that the response plan is focused on health care services and is separate from the new Covid Coordinating Secretariat that was announced on Thursday.
Ethical allocations of scare resources
The response plan contains a section on making decisions while working with scarce resources, such as medevac flights, critical care beds and ventilators.
Those decisions would become particularly sensitive in cases where patients were already medically vulnerable before contracting Covid.
For that purpose, the NWT Scarce Resource Triage Committee was set up to help with decision making.
"We need the ethical framework so people don't act on unconscious bias," said Cook. "The Triage Committee has an Indigenous Elder and ethicist. They would guide triage choices to avoid biases and overcome systemic racism."
Securing resources
Health authorities are trying to obtain all the necessary medical and personal protective equipment (PPE), Cook said, but all other jurisdictions are doing the same, leading to supply shortages.
"We have three ventilators on order that haven't arrived yet," she said.
That would add to the 13 ventilators, including ambulance transport ventilators that the NWT already has, as Cook said in March.
The rush for more resources also means the NWT has yet to receive more GeneXpert and BioFire rapid testing devices.
Cook said a significant announcement would be made in the next week about Covid testing capacity.