A gonorrhea epidemic is here and it might not be treatable.
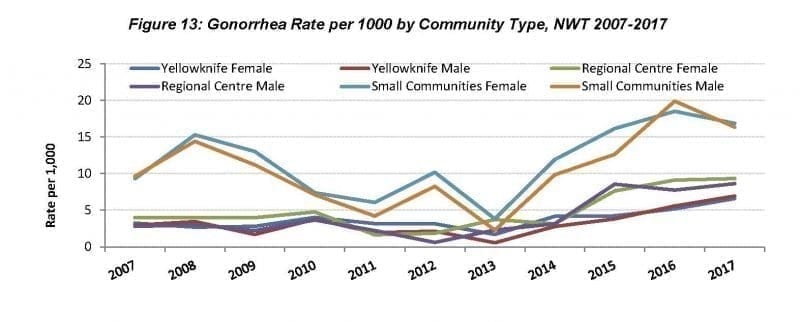
After falling for 20 years, the number of reported cases of gonorrhea has gone up more than 53 percent across Canada over the past 10 years. The NWT is sitting on rates that are more than 18 times the national average, according to the the GNWT.
As of 2015, the last time data was available, 0.6 people out of every 1,000 had gonorrhea across Canada. Numbers from 2016 found that in the NWT, 11 out of every 1,000 people were infected.
Now, the World Health Organization is warning a growing number of strains aren't treatable with antibiotics.
“If you were using the word epidemic I wouldn't quarrel with you,” said chief public health officer Andre Corriveau. “We've had overall a four-time increase since 2013. So we've had a very sharp rise in the last three to four years.”
The territorial government reports the most affected group is women between 15- and 24-years old, and men aged 20 to 29. And while Yellowknife's status as the biggest city in the territory means that the city can claim the highest number of infections, smaller communities have seen a sharper increase in the rate of infection since 2013.
Amy Stitdonk, one of the community health nurses and the manager of continuing care in Fort Simpson says the solution is to get tested.
“These rates are very alarming for the population of the Northwest Territories,” she said. “If they are having unprotected sex with more than one partner, they need to be protecting themselves and they need to be getting themselves tested.”
She said the test, a simple urine sample, is available during nurse visits in smaller communities or at any health centre that has a nursing station with full-time health-care staff. In Yellowknife, testing is available through the STI Nurse at the Yellowknife Primary Care Centre, or any physician or nurse practitioner.
Symptoms might not show up right away, and if they do they can include discharge, pain and a burning or itching sensation. Gonorrhea can also be passed orally and infect the throat. If left untreated, there can be serious consequences, including infertility and an increased risk for HIV. Gonorrhea can also infect the bloodstream and spread to other parts of the body. This can be life threatening.
“We had achieved a lot of success after the HIV epidemic and the safe sex messaging in the 1990s. By 2000 our rates of gonorrhea were almost zero,” said Corriveau. “There's an attitude now that it's not a big deal to get some of these infections because you can get treatment.”
Only, you can't. In July, the World Health Organization released data from 77 countries that found “widespread resistance” to older and cheaper antibiotics, with cases popping up that are untreatable by all known antibiotics.
"The bacteria that cause gonorrhea are particularly smart,” stated Dr. Teodora Wi, a World Health Organization (WHO) medical officer in a news release. “Every time we use a new class of antibiotics to treat the infection, the bacteria evolve to resist them.”
Specifically, WHO data found that between 2009 and 2014, 97 per cent of countries in the study reported gonorrhea strains that were resistant to antibiotic ciprofoxacin, with 81 per cent reporting resistance to antiobiotic azithromycin.
Right now, antiobiotic cephalosoprin is a the last-resort treatment option, but resistance to it has now been reported in more than 50 countries.
There's no super drug waiting in the wings, ready to make its triumphant debut either - WHO reports the pipeline for new antibiotics to combat gonorrhea isn't exactly overflowing, with just three new candidate drugs in various stages of clinical development.
Currently in the NWT, Stitdonk said gonorrhea is most commonly treated with a single-dose antibiotic because Corriveau says “fortunately” untreatable strains haven't popped up in the NWT yet.
“It's still rare, but certainly because of the pattern of transmission and global travel it's not sort of far fetched to think it could spread quite fast around the world if we don't have some kind of a mitigation strategy,” he said. “We have to change the way we communicate about this issue to really convey that there is a risk to your health if you don't get tested regularly and if you end up with an infection that is hard to treat.”